Brain Tumors
Karolinska University Hospital is an OECI-designated comprehensive cancer facility which means it meets the strict standards of the Organisation of European Cancer Institutes. A new era of personalized cancer medicine has emerged, and Karolinska University Hospital is at the forefront of this development, offering the latest diagnostics and treatments for brain tumors, to improve the lives of our patients.
Brain tumors are a heterogeneous group of tumors, where some brain tumors are non-cancerous (benign), and some brain tumors are cancerous (malignant). Brain tumors can begin in the brain (primary brain tumors), or cancer can begin in another part of the body and spread to the brain as a metastasis (secondary brain tumor). Glioblastoma is the most common and aggressive brain tumor that inevitably recurs despite treatment.
Neurosurgery
Pioneers in modern neurosurgery with extensive collaborations worldwide. arrow_right_alt NeurosurgeryOncology
Our goal is to offer world-class cancer care based on every patient's individual needs. arrow_right_alt OncologyNeurology
We receive patients with neurological diseases that require more specialized assessment and care. arrow_right_alt Neurology
Request medical treatment
More information on who can request a medical second opinion or treatment at Karolinska.
Continue
arrow_right_alt
home_health Center
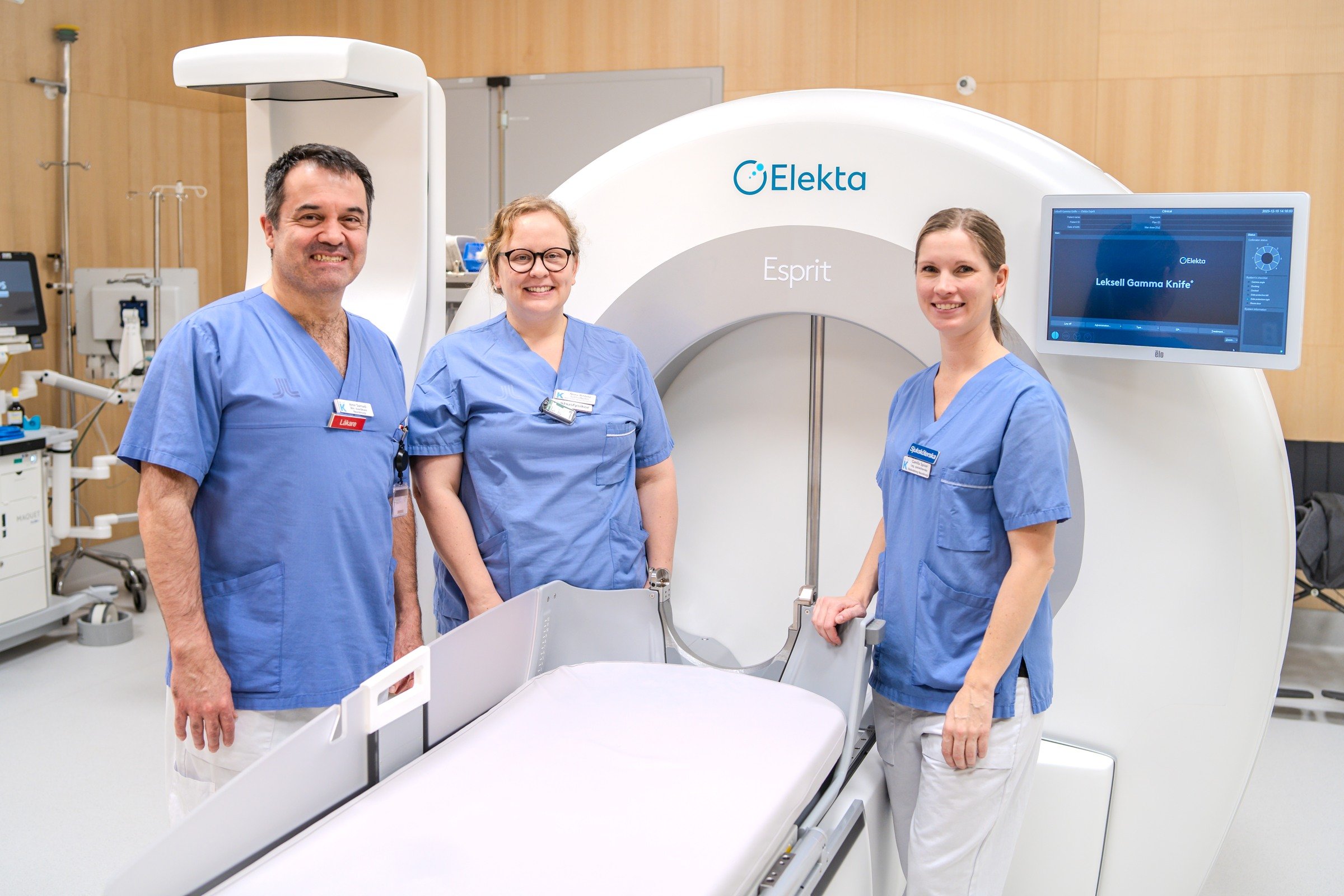
Gamma Knife
arrow_right_alt
Since the invention of the Gamma Knife at Karolinska in the 1960s, we are the only hospital in the world with more than 50 years of experience treating patients with the device.
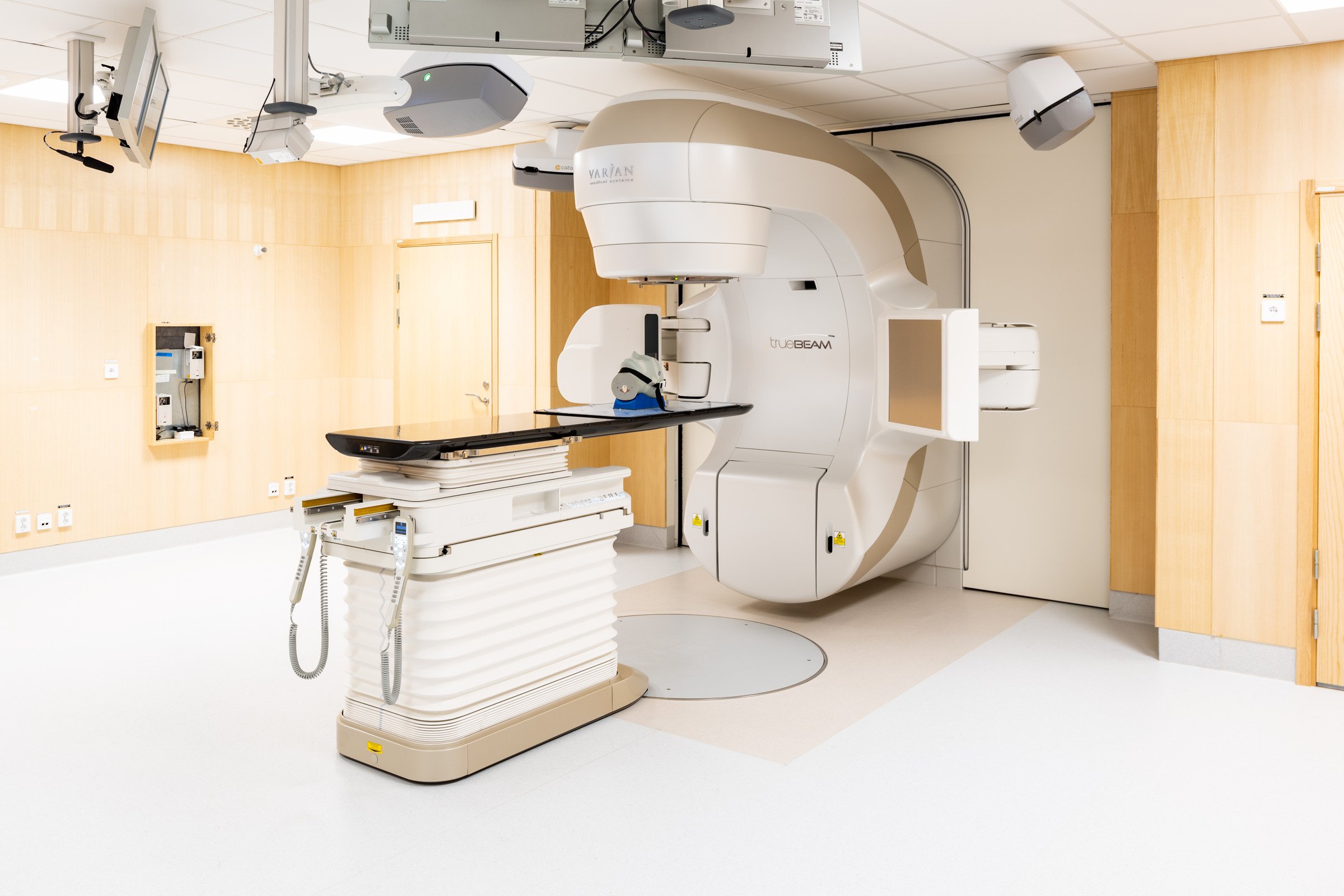
home_health Center
Karolinska Comprehensive Cancer Center
arrow_right_alt
Bringing together cutting-edge research and world-leading expertise